[C.P Chung ten@tenspace.co.kr] Kyung Hee University, led by President Gyun-Tae Han, announced on February 22nd that a joint research team, headed by Professor Eun-Jeong Park from the School of Medicine and Professor Dong-Wan Kim from the College of Engineering at Korea University, led a study on the effects of nanofiber exposure on the respiratory tract. The study results were published in the international toxicology journal, ‘Nanotoxicology’ (IF=5.913).
The study sought to determine whether health changes caused by synthetic microfibers were due to chemical components in the fibers or physical factors. The research team introduced polyethylene microfibers and silk microfibers into the human body through the respiratory system, with the aim of investigating their impact. When the microfibers were administered to the respiratory tract of mice for four weeks, the body weight of female mice exposed to high concentrations of silk microfibers decreased significantly compared to the control group. The number of cells in the alveoli increased in mice administered with microfibers compared to the mouse group not aided with microfibers, regardless of their nature. However, only female mice exposed to silk microfibers exhibited a significant increase in the ratio of neutrophils to eosinophils.
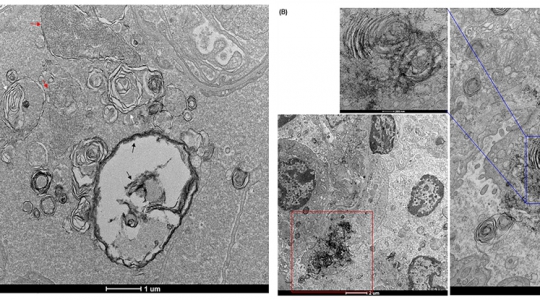
In the lung tissues of mice exposed to polyethylene microfibers and silk microfibers, the research team observed inflammatory cell infiltration into blood vessels, bronchioles, and interstitium, macrophage aggregation in alveoli, degeneration and hypertrophy of arteriolar media, the proliferation of mucous cells, formation of mucous plugs, and histopathological changes such as the appearance of multinucleated giant cells and foamy macrophages. Among the 12 inflammation-related markers involved in these changes, the concentrations of CXCL1 and MCP-1α are involved in the influx of neutrophils and macrophages, and TGF-β, which is involved in the repair of damaged tissues, increased. TGF-β is also a marker closely related to the development of idiopathic pulmonary fibrosis.
The study suggests that synthetic microfibers exposed through the respiratory system can cause immunological and biochemical changes in the blood and induce systemic health effects. Durable synthetic microfibers are less likely to be excreted once ingested into the body, making indoor air management crucial.
Professor Park Eun-Jung, who led the study, emphasized the importance of indoor air management and the care taken when drying laundry at home or using a dryer. More attention should be paid to households with crawling babies or active children or when indoors are dry in winter, as microfibers are more likely to float.
The study received support from the National Research Foundation of Korea and the Institute for Safety Evaluation. Professor Park Eun-Jung was designated as a respiratory safety data center designated by the National Reference Standard Center under the Ministry of Trade, Industry, and Energy in November of last year, furthering her research momentum.